Differences Between Credentialing Privileging And Enrollment Medwave
Credentialing Privileging Enrollment Healthcare Compliance Pillars While credentialing establishes a provider’s qualifications, privileging determines the specific clinical activities a practitioner is allowed to perform within a healthcare facility. Now that you understand credentialing, enrollment, and privileging, you can see how they differ. credentialing focuses on a practitioner’s general qualifications, privileging on their specific abilities, and enrollment on allowing them to serve patients with certain health coverage.

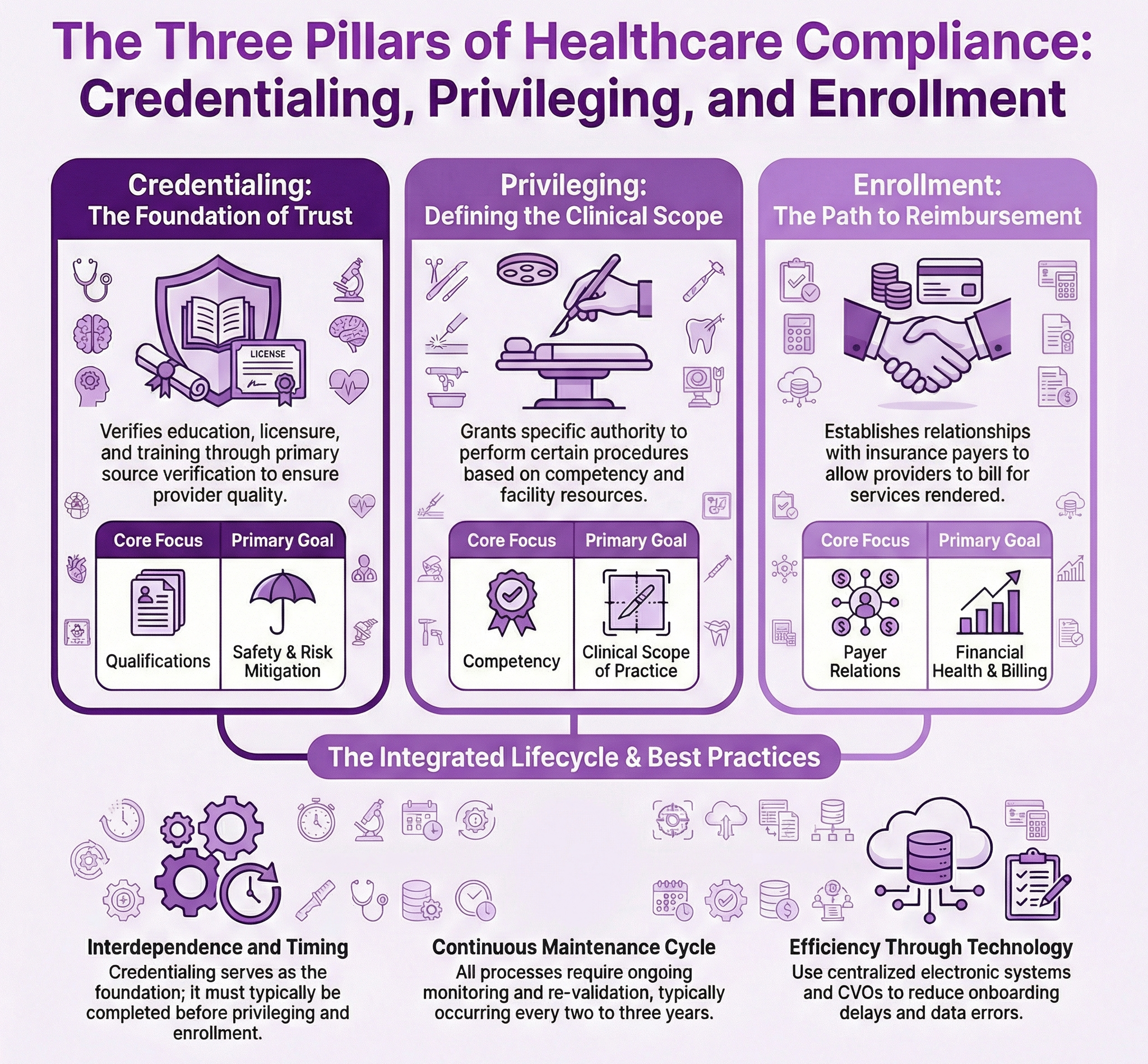
Differences Between Credentialing Privileging And Enrollment Medwave Credentialing assesses if a provider meets institutional requirements for staff inclusion, such as training, board certification, and malpractice event history. in contrast, privileging evaluates a provider's behavior, skills, and procedures within their practice scope at the institution. Among these terms, “credentialing,” “enrollment,” and “privileging” are frequently encountered but are not always clearly understood. this article aims to clarify these concepts, emphasizing their importance in delivering quality healthcare. An infographic of the three pillars of healthcare compliance: credentialing, privileging, and enrollment. Three critical processes play a pivotal role in ensuring the quality, safety, and efficiency of patient care: credentialing, privileging, and enrollment.

Differences Between Credentialing Privileging And Enrollment Medwave An infographic of the three pillars of healthcare compliance: credentialing, privileging, and enrollment. Three critical processes play a pivotal role in ensuring the quality, safety, and efficiency of patient care: credentialing, privileging, and enrollment. In the healthcare industry, the terms “credentialing” and “privileging” are often used interchangeably, but they actually serve distinct and critical roles. failing to understand the differences between these two processes can lead to administrative errors, compliance issues, and even patient safety concerns. Enrollment is the process of joining an insurance network to get paid. if the doctors are privileged and credentialed, they still cannot get paid by the insurance companies until they get enrolled. Terms like credentialing, privileging, and enrollment are often used interchangeably. however, they represent distinct processes with unique implications for healthcare providers and facilities. understanding these differences is crucial for smooth operations and a compliant revenue cycle. Any physician or other practitioner seeking to bill, independently, for their services must navigate credentialling, privileging, and network enrollment processes. while these three processes are often referred to as one process, they are three distinct, yet interwoven, procedures.
Comments are closed.