Credentialing Vs Enrollment Whats The Difference

The Difference Between Payer Enrollment And Credentialing Credentialing proves a provider is qualified; enrollment ensures that qualification is recognized by insurers like medicare, medicaid, and commercial health plans. Understanding the key differences between physician credentialing and payer enrollment processes, timelines, and requirements for successful practice operations.

Credentialing Checklist Credentialing Enrollment Solutions Discover the difference between healthcare provider enrollment and credentialing and see why they're both vital. learn more. Credentialing is about verifying qualifications; enrollment is about joining a payer network. a provider can be credentialed but not enrolled—meaning they are qualified, but still not able to bill certain payers. What is the difference between credentialing and enrollment? credentialing verifies a provider’s qualifications and history, while enrollment registers them with insurance networks to submit claims. Provider credentialing and provider enrollment are both important steps in becoming a participating healthcare provider in an insurance network. while these terms are often used interchangeably, they actually refer to different steps in the process of becoming a participating provider.
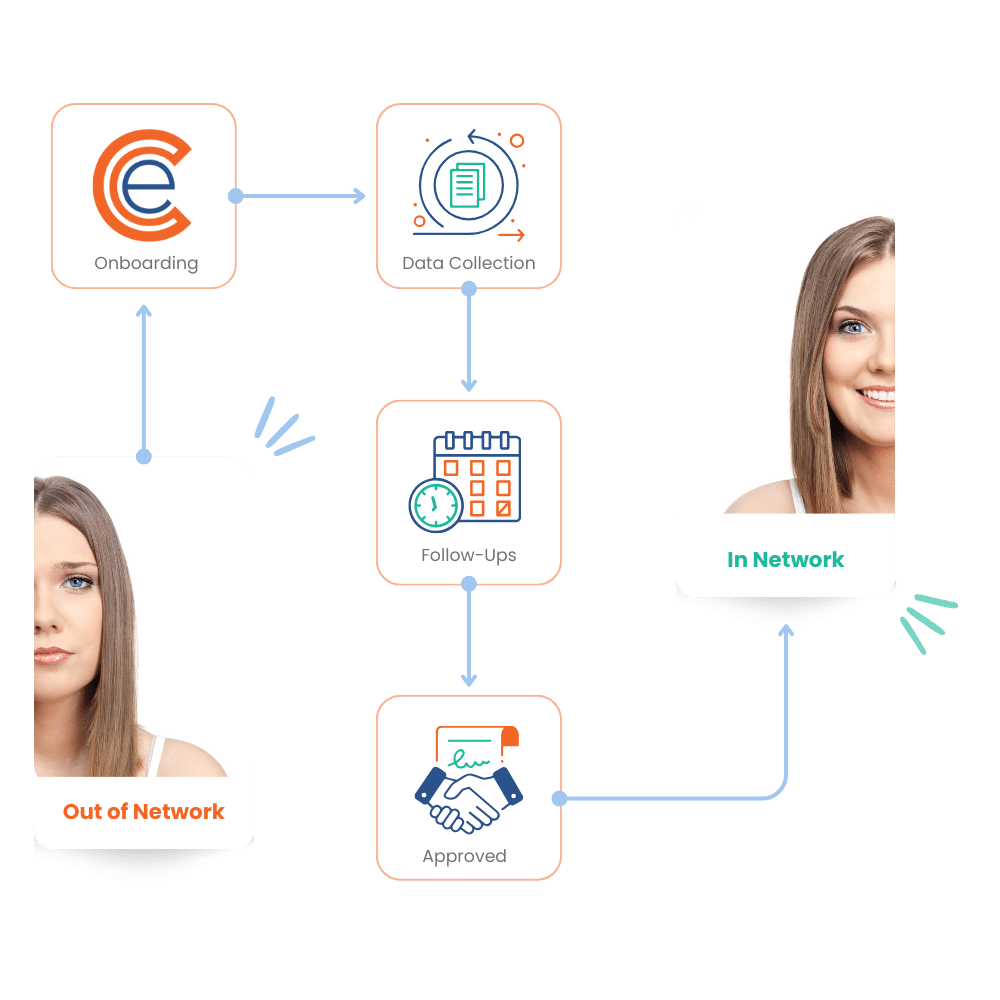
Credentialing Enrollment Solutions Simplifying The Path To What is the difference between credentialing and enrollment? credentialing verifies a provider’s qualifications and history, while enrollment registers them with insurance networks to submit claims. Provider credentialing and provider enrollment are both important steps in becoming a participating healthcare provider in an insurance network. while these terms are often used interchangeably, they actually refer to different steps in the process of becoming a participating provider. Once credentialing is complete, provider enrollment ensures a provider can bill insurers and receive reimbursement. while credentialing proves a provider’s qualifications, enrollment makes those credentials recognized by insurance payers, including medicare, medicaid, and commercial health plans. Provider enrollment and credentialing involve verifying a provider's qualifications and linking them to payers to ensure clinical competency before billing. What is the difference between credentialing and provider enrollment? credentialing is the internal process of verifying a provider’s qualifications — confirming their education, licensure, certifications, and clinical history through primary source verification. Understand the difference between credentialing and enrollment in healthcare and why both are critical for compliance and reimbursements.

Credentialing Enrollment Privileging Differences Explained Bellmedex Once credentialing is complete, provider enrollment ensures a provider can bill insurers and receive reimbursement. while credentialing proves a provider’s qualifications, enrollment makes those credentials recognized by insurance payers, including medicare, medicaid, and commercial health plans. Provider enrollment and credentialing involve verifying a provider's qualifications and linking them to payers to ensure clinical competency before billing. What is the difference between credentialing and provider enrollment? credentialing is the internal process of verifying a provider’s qualifications — confirming their education, licensure, certifications, and clinical history through primary source verification. Understand the difference between credentialing and enrollment in healthcare and why both are critical for compliance and reimbursements.

Credentialing Enrollment Privileging Differences Explained Bellmedex What is the difference between credentialing and provider enrollment? credentialing is the internal process of verifying a provider’s qualifications — confirming their education, licensure, certifications, and clinical history through primary source verification. Understand the difference between credentialing and enrollment in healthcare and why both are critical for compliance and reimbursements.

Credentialing Enrollment Privileging Differences Explained Bellmedex
Comments are closed.