Introduction Qpp Mips Advanced Apms
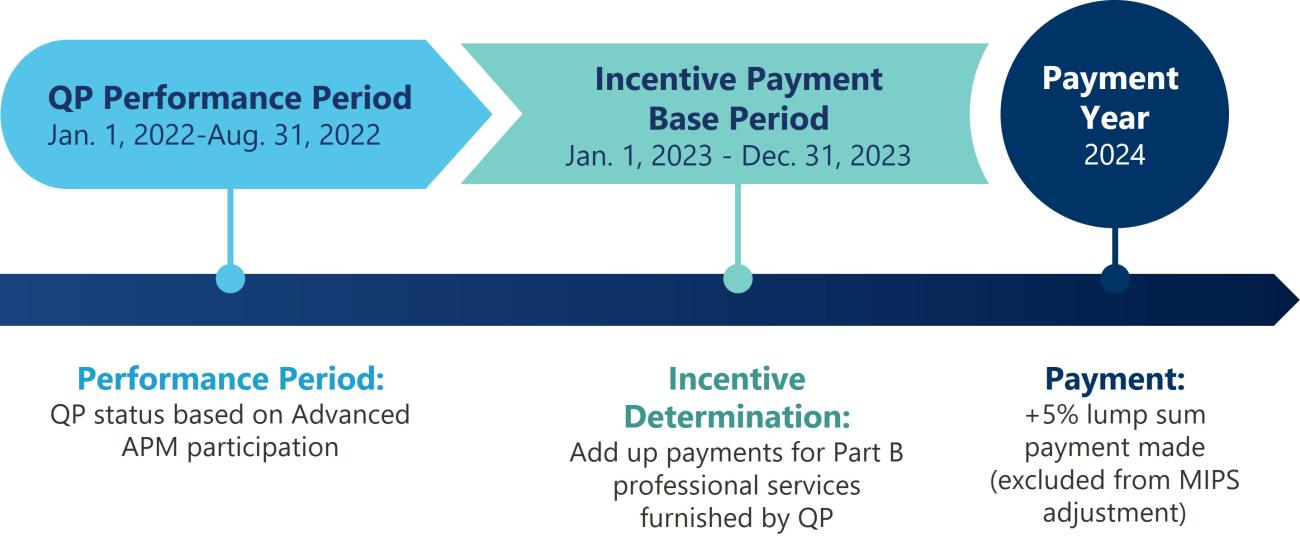
Advanced Apms Qpp Advanced alternative payment models (apms) are one track of the quality payment program that offer incentives for meeting participation thresholds based on your levels of payments or patients through advanced apms. if you achieve these thresholds, you become a qualifying apm participant (qp). About press copyright contact us creators advertise developers terms privacy policy & safety how works test new features nfl sunday ticket © 2025 google llc.
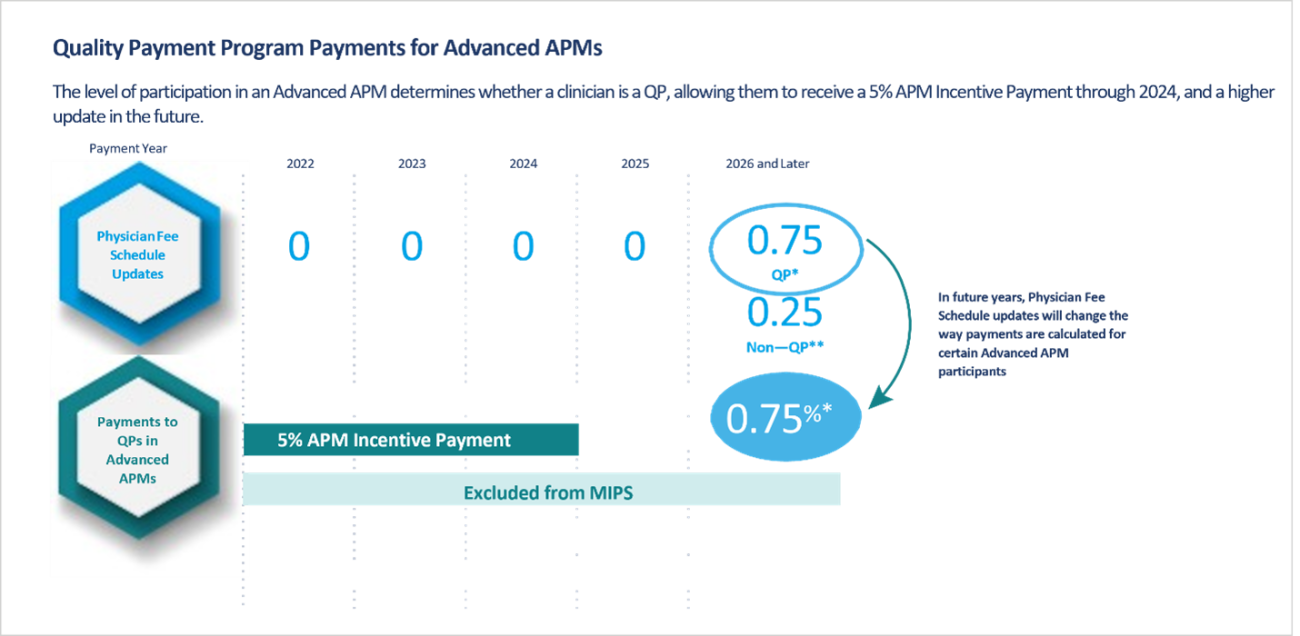
Advanced Apms Qpp Macra established two separate frameworks within the qpp: mips and advanced apms. these tracks encourage healthcare providers to focus on delivering better patient outcomes while minimizing unnecessary spending. The quality payment plan (qpp) has two paths that you could take for reporting for your reimbursements from cms – mips, which has a few options under that path; and the advanced apms. The quality payment program (qpp) provides medicare providers with three primary participation tracks: the merit based incentive payment system (mips), advanced alternative payment models (apms), and mips value pathways (mvps). What is the merit based incentive payment system? the merit based incentive payment system (mips) is one way to participate in the quality payment program (qpp). under mips, we evaluate your performance across multiple categories that drive improved quality and value in our healthcare system.
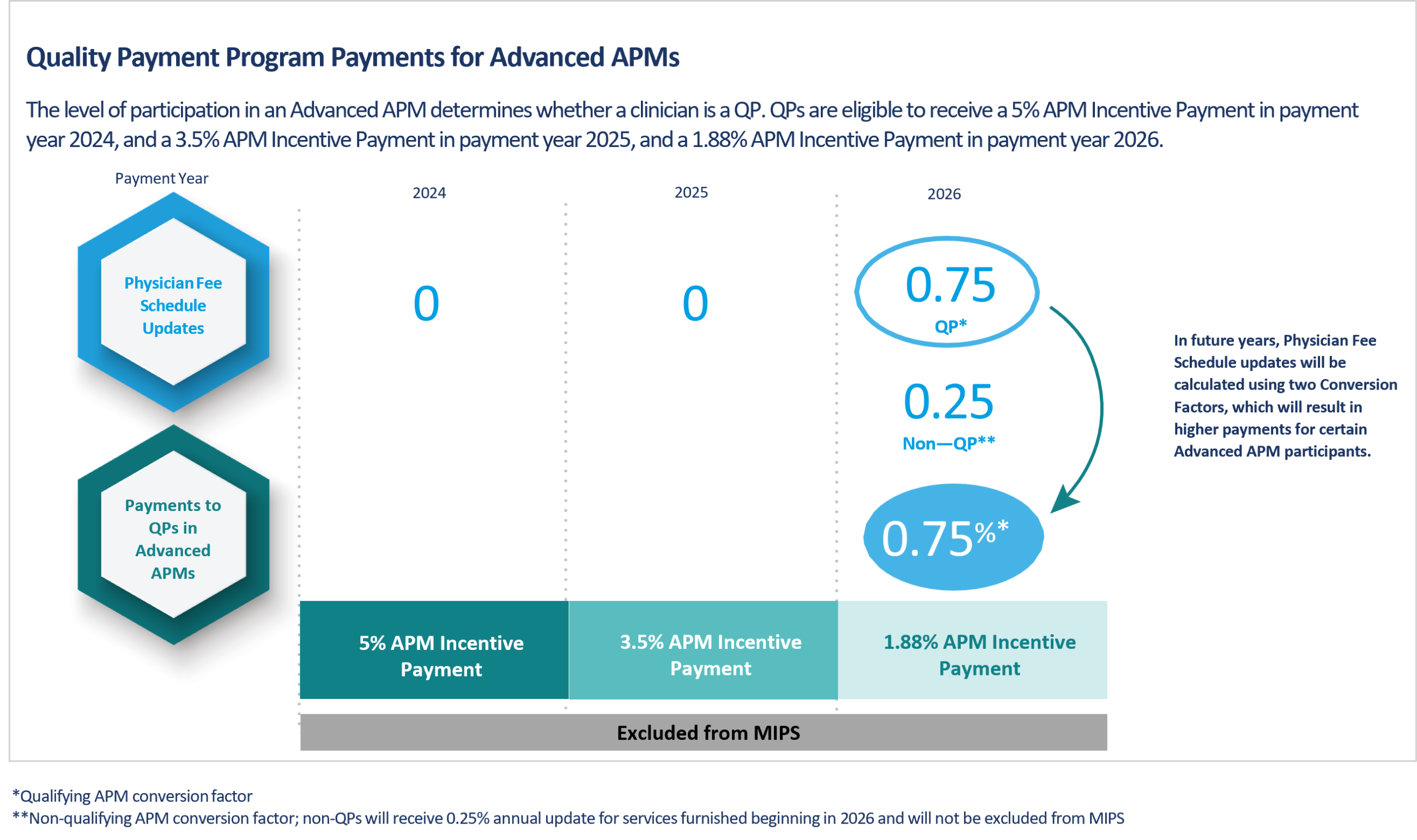
Qpp The quality payment program (qpp) provides medicare providers with three primary participation tracks: the merit based incentive payment system (mips), advanced alternative payment models (apms), and mips value pathways (mvps). What is the merit based incentive payment system? the merit based incentive payment system (mips) is one way to participate in the quality payment program (qpp). under mips, we evaluate your performance across multiple categories that drive improved quality and value in our healthcare system. Clinicians can participate in the qpp through either the merit based incentive payment system (mips) — earning payment adjustments based on performance for services provided to medicare patients — or advanced apms, where they earn payment for delivering high quality, high value care. Advanced alternative payment models (apms): if you decide to take part in an advanced apm, you may earn a medicare incentive payment for sufficiently participating in an innovative payment model. get fact sheets from the qpp resource library. attend or replay webinars. Mips apm participants may choose to report mips through the apm performance pathway (app). the app is an optional mips reporting and scoring pathway for mips eligible clinicians, groups and apm entities that also participate in mips apms, except for shared savings program acos that are required to report through the app. Some of these apms qualify as advanced apms under the quality payment program, or qpp. advanced apms let clinicians earn more rewards in exchange for taking on risk related to delivery of high quality, cost efficient care.

Mips Apms 2019 Qpp Models The Valletta Group Clinicians can participate in the qpp through either the merit based incentive payment system (mips) — earning payment adjustments based on performance for services provided to medicare patients — or advanced apms, where they earn payment for delivering high quality, high value care. Advanced alternative payment models (apms): if you decide to take part in an advanced apm, you may earn a medicare incentive payment for sufficiently participating in an innovative payment model. get fact sheets from the qpp resource library. attend or replay webinars. Mips apm participants may choose to report mips through the apm performance pathway (app). the app is an optional mips reporting and scoring pathway for mips eligible clinicians, groups and apm entities that also participate in mips apms, except for shared savings program acos that are required to report through the app. Some of these apms qualify as advanced apms under the quality payment program, or qpp. advanced apms let clinicians earn more rewards in exchange for taking on risk related to delivery of high quality, cost efficient care.
Comments are closed.