1st Credentialing Preparing For Payor Enrollment
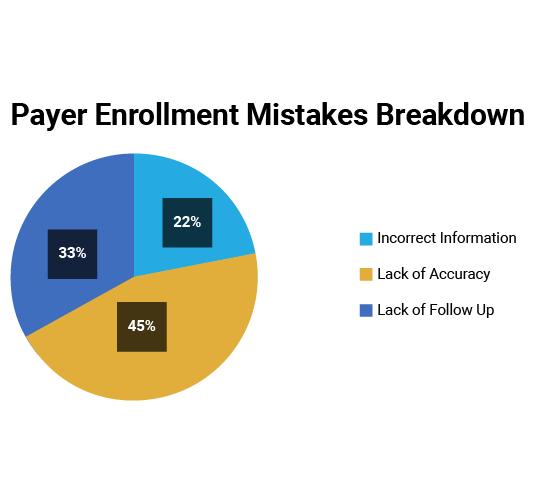
Payor Enrollment Education Archives 1ë áµ Credentialing Our credentialing experts are here to help you assess exactly which solutions you need to put you on the right track. 1ˢᵗ credentialing includes payor enrollment for all insurance networks. Credentialing and payer enrollment from start to finish: caqh setup, payer timelines, re credentialing, and revenue impact of delays.

Payor Enrollment Education Archives 1ë áµ Credentialing In this guide, we’ll break down how credentialing and payer enrollment work, where they differ, and how to manage both more efficiently to avoid unnecessary delays and revenue loss. Complete provider credentialing guide covering process, requirements, timelines, documents, and payer enrollment steps for healthcare providers and practices. Before enrollment is approved, many payers require you to complete a credentialing step. fill in all requested fields, upload clear documents, and verify that names, addresses, and dates are consistent with your other materials. Keep in mind, unless otherwise allowed by state regulations, providers must be approved through both the credentialing and contracting processes before consideration and the ability to submit claims as an approved network provider.

Speed Up Payor Enrollment 5 Essential Credentialing Strategies Before enrollment is approved, many payers require you to complete a credentialing step. fill in all requested fields, upload clear documents, and verify that names, addresses, and dates are consistent with your other materials. Keep in mind, unless otherwise allowed by state regulations, providers must be approved through both the credentialing and contracting processes before consideration and the ability to submit claims as an approved network provider. Step by step credentialing and payer enrollment. caqh, pecos, commercial contracts, timelines, and kpis, handled by next rcm’s credentialing services. This course serves as a practical, job ready introduction to provider credentialing and payer enrollment —ideal if you want to speed approvals, reduce denials, and support a healthy revenue cycle. Prevents credentialing delays rapidly increases enrollment and reimbursement in the network. lessens recurrent requests of the payers to provide information. allow all payers in the first place. when initially registering caqh, approve all the insurance companies you intend to join. this enables simultaneous rather than sequential credentialing. To initiate credentialing, the provider must submit a credentialing application and supporting documents to each payor they wish to enroll with. the process may take several weeks or months, depending on the payor’s policies and procedures.

Differences Between Payor Enrollment And Credentialing Step by step credentialing and payer enrollment. caqh, pecos, commercial contracts, timelines, and kpis, handled by next rcm’s credentialing services. This course serves as a practical, job ready introduction to provider credentialing and payer enrollment —ideal if you want to speed approvals, reduce denials, and support a healthy revenue cycle. Prevents credentialing delays rapidly increases enrollment and reimbursement in the network. lessens recurrent requests of the payers to provide information. allow all payers in the first place. when initially registering caqh, approve all the insurance companies you intend to join. this enables simultaneous rather than sequential credentialing. To initiate credentialing, the provider must submit a credentialing application and supporting documents to each payor they wish to enroll with. the process may take several weeks or months, depending on the payor’s policies and procedures.
Understanding The Differences Between Payor Enrollment And Prevents credentialing delays rapidly increases enrollment and reimbursement in the network. lessens recurrent requests of the payers to provide information. allow all payers in the first place. when initially registering caqh, approve all the insurance companies you intend to join. this enables simultaneous rather than sequential credentialing. To initiate credentialing, the provider must submit a credentialing application and supporting documents to each payor they wish to enroll with. the process may take several weeks or months, depending on the payor’s policies and procedures.

5 Ways To Accelerate Payor Enrollment Credentialing Bellmedex
Comments are closed.