Severe Left Ventricular Dysfunction Dcmp Echo Clip Youtube

Echo Lv Diastolic Dysfunction Youtube #dcmp #echo severe left ventricular dysfunction dcmp echo clip. Evaluation of lv mechanical dyssynchrony in dcm patients with heart failure (hf), severe lv dysfunction, and left bundle branch block (lbbb) has been widely studied and principally applied to identify potential responders to crt (clip 5.9).

Dcmp Severe Lv Dysfunction Youtube It is characterised by chamber enlargement and contractile dysfunction of the left ventricle in the absence of chronic pressure and or volume overload. although not essential for diagnosis, the right ventricle may similarly be affected. This video clip demonstrates a dilated and globally hypokinetic left ventricle with a large, echodense thrombus adherent to the lv apex — a classic finding in advanced dcmp with severe lv dysfunction. M mode echocardiogram is commonly used to measure left ventricular dimensions and ejection fraction. ejection fraction is indicative of the left ventricular systolic function. 🔹 pathophysiology in dcmp, severe systolic dysfunction leads to stasis of blood in lv apex, promoting thrombus formation — part of virchow’s triad (stasis, endothelial injury, hypercoagulability). 🔹 clinical significance risk of systemic embolization (stroke, limb ischemia) requires anticoagulation and treatment of underlying lv.

Dcm With Severe Lv Dysfunction Youtube M mode echocardiogram is commonly used to measure left ventricular dimensions and ejection fraction. ejection fraction is indicative of the left ventricular systolic function. 🔹 pathophysiology in dcmp, severe systolic dysfunction leads to stasis of blood in lv apex, promoting thrombus formation — part of virchow’s triad (stasis, endothelial injury, hypercoagulability). 🔹 clinical significance risk of systemic embolization (stroke, limb ischemia) requires anticoagulation and treatment of underlying lv. The likelihood of developing a left bundle branch block increases with the severity of left ventricular dysfunction. more than one half of patients with severely reduced left ventricular function have a left bundle branch block. Today, we explore the echocardiography essentials course with a video on how to recognize normal, hyperkinetic and hypokinetic function of the left ventricle with the help of transthoracic echo. The risk of sudden cardiac arrest and sustained ventricular tachycardia is high among these individuals, regardless of the severity of left ventricular dysfunction. also, a family history of ventricular arrhythmias predicts a high risk of arrhythmogenic dcm. Some cases of dcm with severe systolic dysfunction (left ventricular ejection fraction ≤ 35%) and wide qrs complex remain symptomatic, with chronic heart failure (nyha class ii–iv) despite optimal medical treatment.
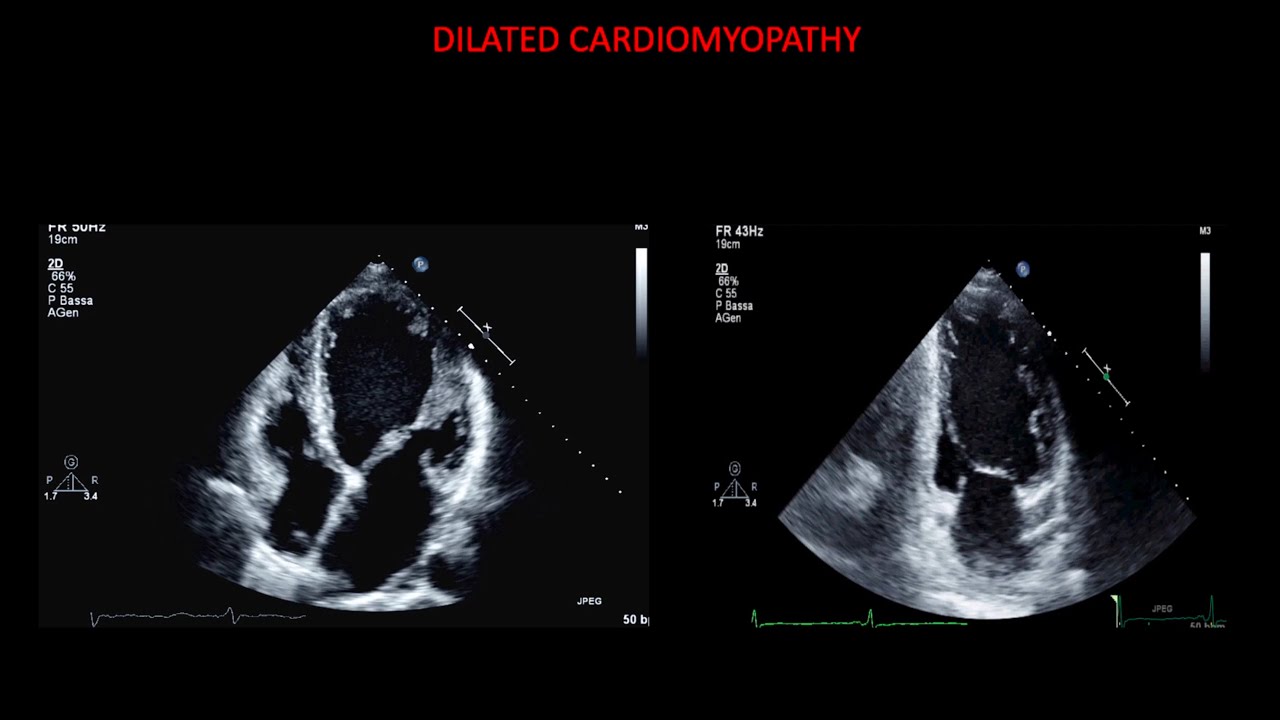
Echocardiography In Dilated Cardiomyopathy Youtube The likelihood of developing a left bundle branch block increases with the severity of left ventricular dysfunction. more than one half of patients with severely reduced left ventricular function have a left bundle branch block. Today, we explore the echocardiography essentials course with a video on how to recognize normal, hyperkinetic and hypokinetic function of the left ventricle with the help of transthoracic echo. The risk of sudden cardiac arrest and sustained ventricular tachycardia is high among these individuals, regardless of the severity of left ventricular dysfunction. also, a family history of ventricular arrhythmias predicts a high risk of arrhythmogenic dcm. Some cases of dcm with severe systolic dysfunction (left ventricular ejection fraction ≤ 35%) and wide qrs complex remain symptomatic, with chronic heart failure (nyha class ii–iv) despite optimal medical treatment.
Comments are closed.