Provider Credentialing

Medical Billing Services This comprehensive guide covers everything healthcare providers need to know about the credentialing process, documentation requirements, and best practices for successful applications. Provider credentialing is a systematic process used by healthcare organizations to verify and evaluate the qualifications, competence, and professional background of healthcare providers.

Simplifying The Provider Credentialing Process Prombs Provider credentialing is the systematic verification of a healthcare provider’s qualifications, including education, training, licensure, certifications, and practice history. this meticulous process serves as the foundation for patient safety, quality care, and organizational integrity. Learn what credentialing is, why it is important, and how to navigate it step by step. find out how intelix credentialing can help you simplify and speed up the process with automated tools and features. Credentialing is a vital process for healthcare institutions. in simple terms, it is the process of assessing a healthcare provider's academic qualifications and clinical practice history. Provider credentialing is the formal process of verifying a healthcare provider’s qualifications, education, licensure, and professional background. it’s carried out by healthcare organizations, insurance payers, and regulators to confirm that a provider can legally and safely deliver care.

What Are The Requirements Of Provider Credentialing Credentialing Credentialing is a vital process for healthcare institutions. in simple terms, it is the process of assessing a healthcare provider's academic qualifications and clinical practice history. Provider credentialing is the formal process of verifying a healthcare provider’s qualifications, education, licensure, and professional background. it’s carried out by healthcare organizations, insurance payers, and regulators to confirm that a provider can legally and safely deliver care. All office based physicians or professional providers who participate in our networks are required to complete a credentialing process prior to acceptance. review the tx initial credentialing checklist to ensure you have all information needed. provider rights. Provider credentialing is a multistep process healthcare systems and plans use to verify healthcare providers' qualifications and competency before granting network inclusion or clinical privileges. this process ensures that clinicians are vetted and compliant with state and federal regulations. Keep it simple. go with the experts at getting your provider credentialing and enrollments done. we help independent providers, groups, or organizations of any size. great pricing and excellent outcomes. our sevices are available nationwide. Provider credentialing is the formal process by which healthcare organizations, hospitals, and insurance payers verify that a clinician possesses the education, training, licensure, and professional history required to deliver patient care and bill for services.

What Is Provider Credentialing In The Us Healthcare System All office based physicians or professional providers who participate in our networks are required to complete a credentialing process prior to acceptance. review the tx initial credentialing checklist to ensure you have all information needed. provider rights. Provider credentialing is a multistep process healthcare systems and plans use to verify healthcare providers' qualifications and competency before granting network inclusion or clinical privileges. this process ensures that clinicians are vetted and compliant with state and federal regulations. Keep it simple. go with the experts at getting your provider credentialing and enrollments done. we help independent providers, groups, or organizations of any size. great pricing and excellent outcomes. our sevices are available nationwide. Provider credentialing is the formal process by which healthcare organizations, hospitals, and insurance payers verify that a clinician possesses the education, training, licensure, and professional history required to deliver patient care and bill for services.

Understanding Provider Credentialing Process Keep it simple. go with the experts at getting your provider credentialing and enrollments done. we help independent providers, groups, or organizations of any size. great pricing and excellent outcomes. our sevices are available nationwide. Provider credentialing is the formal process by which healthcare organizations, hospitals, and insurance payers verify that a clinician possesses the education, training, licensure, and professional history required to deliver patient care and bill for services.
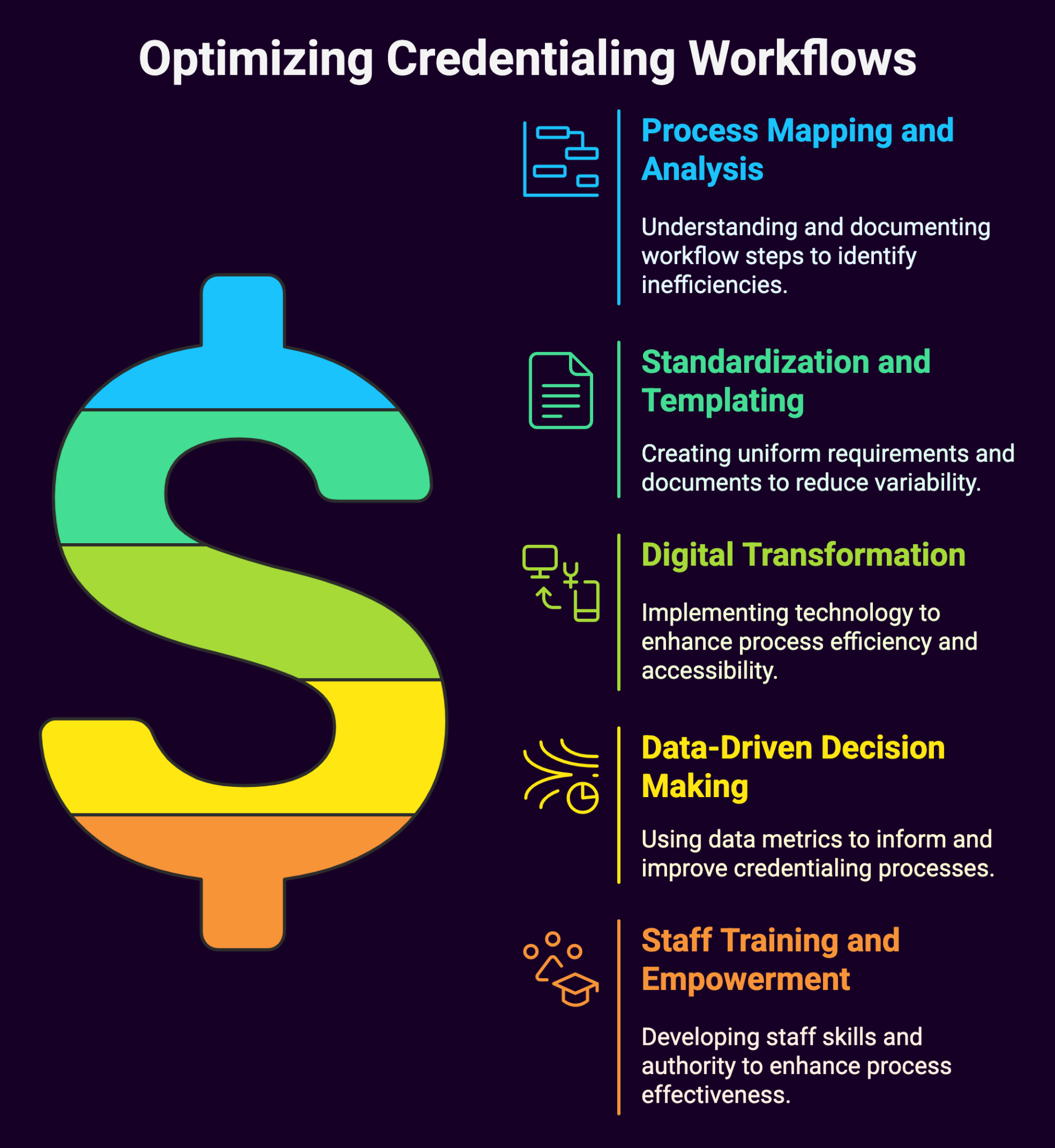
Provider Credentialing Workflow Optimization Medwave
Comments are closed.