Prior Authorization

Prior Authorization Explained A Comprehensive Guide Prior authorization in health care is a requirement that a healthcare provider (such as your primary care physician or a hospital) gets approval from your insurance plan before prescribing you medication or doing a medical procedure. A prior authorization (pa) is a type of permission a healthcare provider needs to get from your health insurance. if your insurance approves it, that means they’ll pay for the care your provider requested.
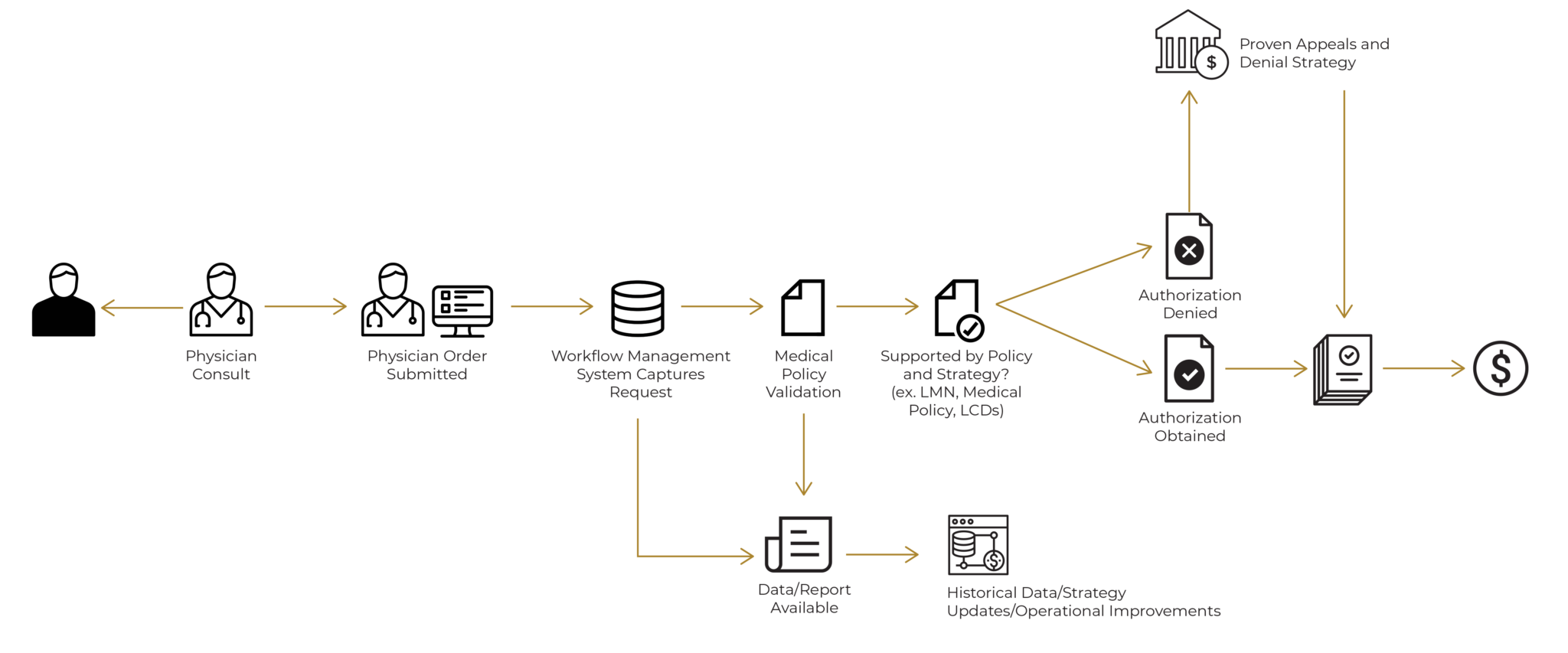
Prior Authorization Services Legion Healthcare Partners Prior authorization is the approval from your health insurance that may be required for a service, treatment, or prescription to be covered by your plan if it's not an emergency. Prior authorization is where some treatments and medications need approval from your health insurance carrier before you receive care. prior authorization is usually required if you need a complex treatment or prescription. your health plan won’t pay for it without approval. Learn how the prior authorization process works in medical billing, why pa denials happen, and how to get prior authorization approved the first time. Prior authorization is an approval of coverage from your insurance company — not your healthcare professional. it’s a restriction put in place to determine whether or not they will pay for certain medications.

Healthcare Prior Authorization Automation Billingparadise Learn how the prior authorization process works in medical billing, why pa denials happen, and how to get prior authorization approved the first time. Prior authorization is an approval of coverage from your insurance company — not your healthcare professional. it’s a restriction put in place to determine whether or not they will pay for certain medications. Prior authorization, also known as preauthorization, preapproval, or precertification, is a process where a healthcare provider must get approval from your health insurance company before insurance will cover a prescribed medication, procedure, or treatment. In medical billing, prior authorization is a process of getting approval from health insurance companies for certain services before treating patients. it could be the prescription, drugs, medications or high cost of treatments. the process is also known as a pre authorization, pre approval or pre certification. Find prior authorization resources to support reform, improve practice efficiency and provide data to highlight the need for change. Prior authorization is when health plans review and approve medical services before they are provided. learn how it works, what services require it, and how it is regulated by the affordable care act and cms.

Healthcare Prior Authorization Automation Billingparadise Prior authorization, also known as preauthorization, preapproval, or precertification, is a process where a healthcare provider must get approval from your health insurance company before insurance will cover a prescribed medication, procedure, or treatment. In medical billing, prior authorization is a process of getting approval from health insurance companies for certain services before treating patients. it could be the prescription, drugs, medications or high cost of treatments. the process is also known as a pre authorization, pre approval or pre certification. Find prior authorization resources to support reform, improve practice efficiency and provide data to highlight the need for change. Prior authorization is when health plans review and approve medical services before they are provided. learn how it works, what services require it, and how it is regulated by the affordable care act and cms.

Healthcare Prior Authorization Automation Billingparadise Find prior authorization resources to support reform, improve practice efficiency and provide data to highlight the need for change. Prior authorization is when health plans review and approve medical services before they are provided. learn how it works, what services require it, and how it is regulated by the affordable care act and cms.
Comments are closed.