Pocus For Lv Systolic Function
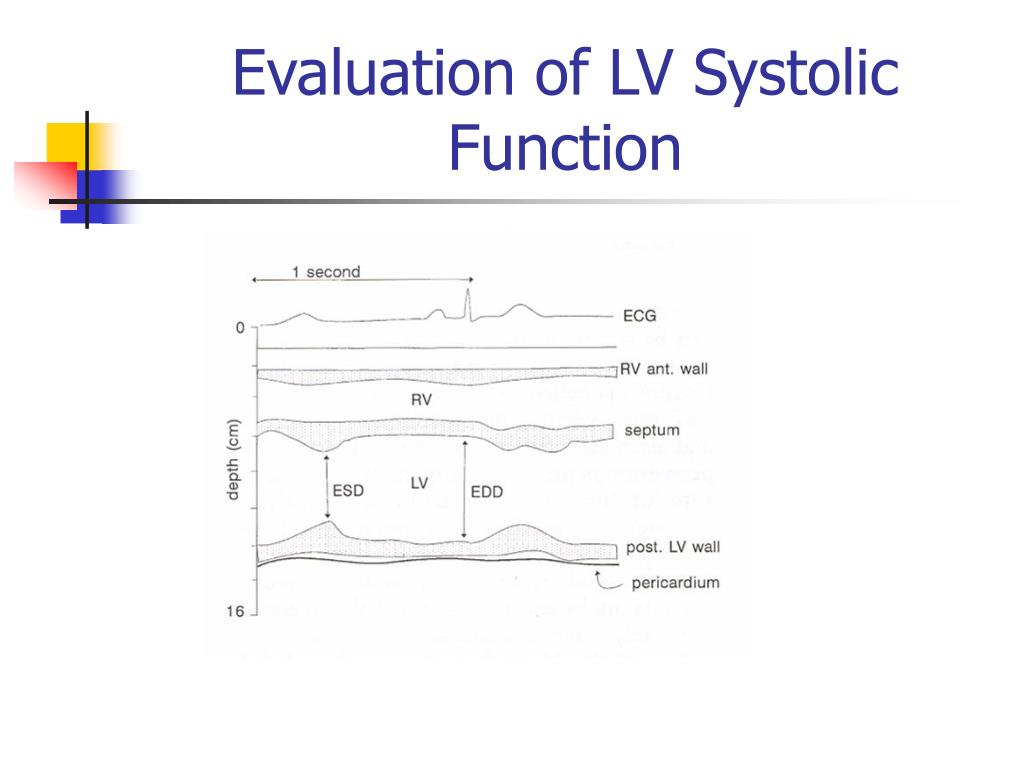
What Does Normal Lv Systolic Function Mean Sema Data Co Op In this post, we will show you the most common qualitative and quantitative approaches to assess left ventricular ejection fraction (lvef) using point of care ultrasound (pocus) and bedside echocardiography to assess the systolic function of your patients. Learn the different methods used to evaluate the ejection fraction of the left ventricle and use pattern recognition to identify grossly abnormal function.

Lv Systolic Function Pptx This method is widely used because it provides a reliable and reproducible assessment of lv function while minimizing geometric assumptions about ventricular shape. In this chapter, the authors will describe how to use pocus to estimate cardiac output non invasively which would be pivotal in the diagnosis and management of cardiogenic shock. myocardial. Basic cardiac point of care ultrasound (pocus) focused cardiac ultrasound (focus) often reveals incidental findings. consider a patient with dyspnea in whom focus reveals left ventricular (lv) hypertrophy, calcified valves, and pericardial effusion but “normal” lv systolic function. In this video, you’ll learn how to assess left ventricular (lv) systolic function using the epss (e point septal separation) method — one of the fastest and most reliable bedside pocus techniques.
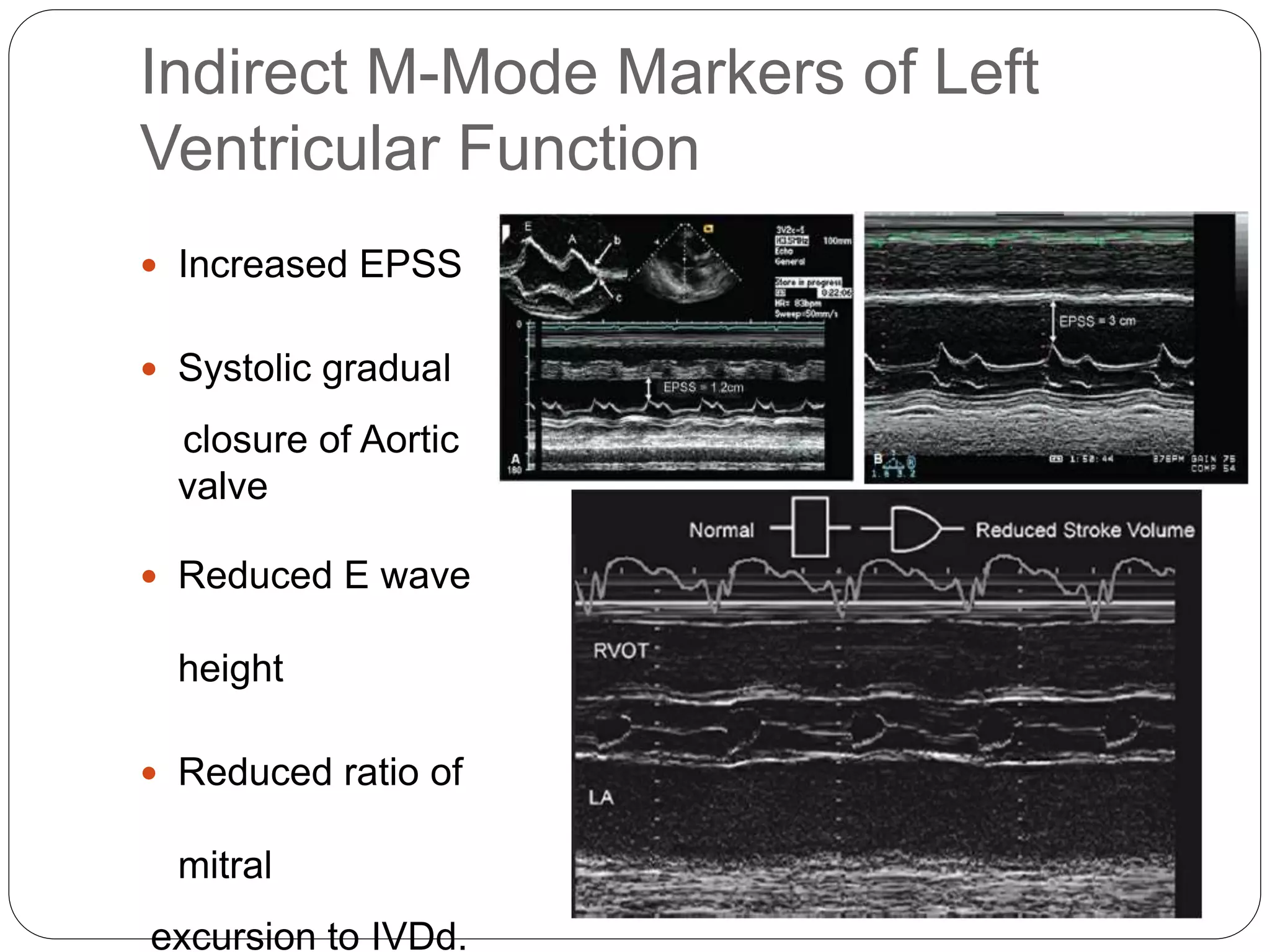
Lv Systolic Function Pptx Basic cardiac point of care ultrasound (pocus) focused cardiac ultrasound (focus) often reveals incidental findings. consider a patient with dyspnea in whom focus reveals left ventricular (lv) hypertrophy, calcified valves, and pericardial effusion but “normal” lv systolic function. In this video, you’ll learn how to assess left ventricular (lv) systolic function using the epss (e point septal separation) method — one of the fastest and most reliable bedside pocus techniques. Currently commercially available pocus devices provide acceptable image quality for focused cardiac assessment and can integrate ai guidance for optimal image acquisition and automated lv function or valvular assessment, which enhances feasibility in patient healthcare environment. After systolic contraction, when most of the blood has been pumped out through the aortic valve (normal ejection fraction of 60%), the relative pressure in the left ventricle is low. in a normal heart at the end of systole, we know the left ventricular pressure is relatively low. This review proposes a pocus approach designed to integrate different qualitative and semi quantitative measurements of lv systolic function, to improve the proficiency in cardiac. In this chapter, the authors will describe how to use pocus to estimate cardiac output non invasively which would be pivotal in the diagnosis and management of cardiogenic shock.
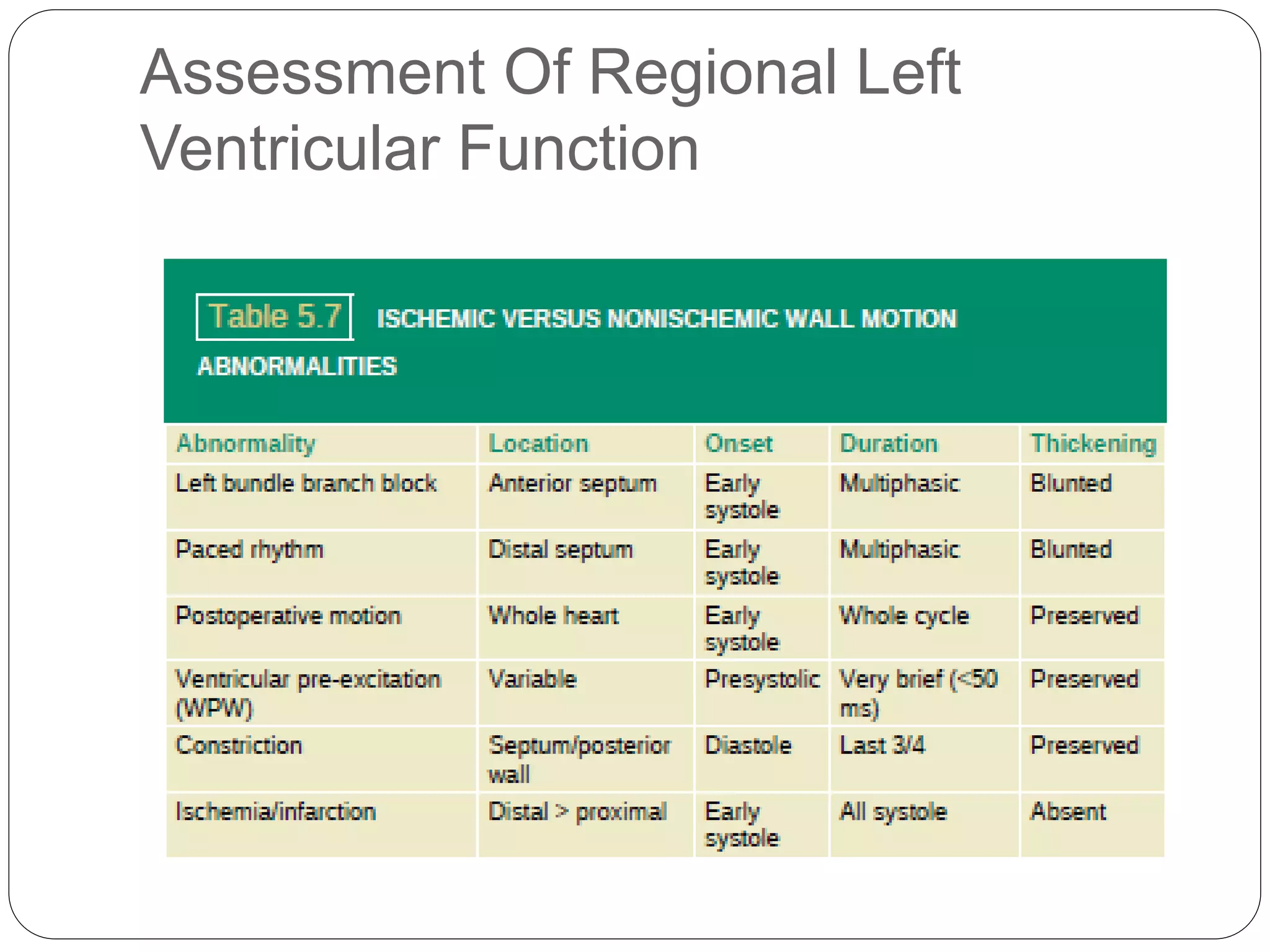
Lv Systolic Function Pptx Currently commercially available pocus devices provide acceptable image quality for focused cardiac assessment and can integrate ai guidance for optimal image acquisition and automated lv function or valvular assessment, which enhances feasibility in patient healthcare environment. After systolic contraction, when most of the blood has been pumped out through the aortic valve (normal ejection fraction of 60%), the relative pressure in the left ventricle is low. in a normal heart at the end of systole, we know the left ventricular pressure is relatively low. This review proposes a pocus approach designed to integrate different qualitative and semi quantitative measurements of lv systolic function, to improve the proficiency in cardiac. In this chapter, the authors will describe how to use pocus to estimate cardiac output non invasively which would be pivotal in the diagnosis and management of cardiogenic shock.
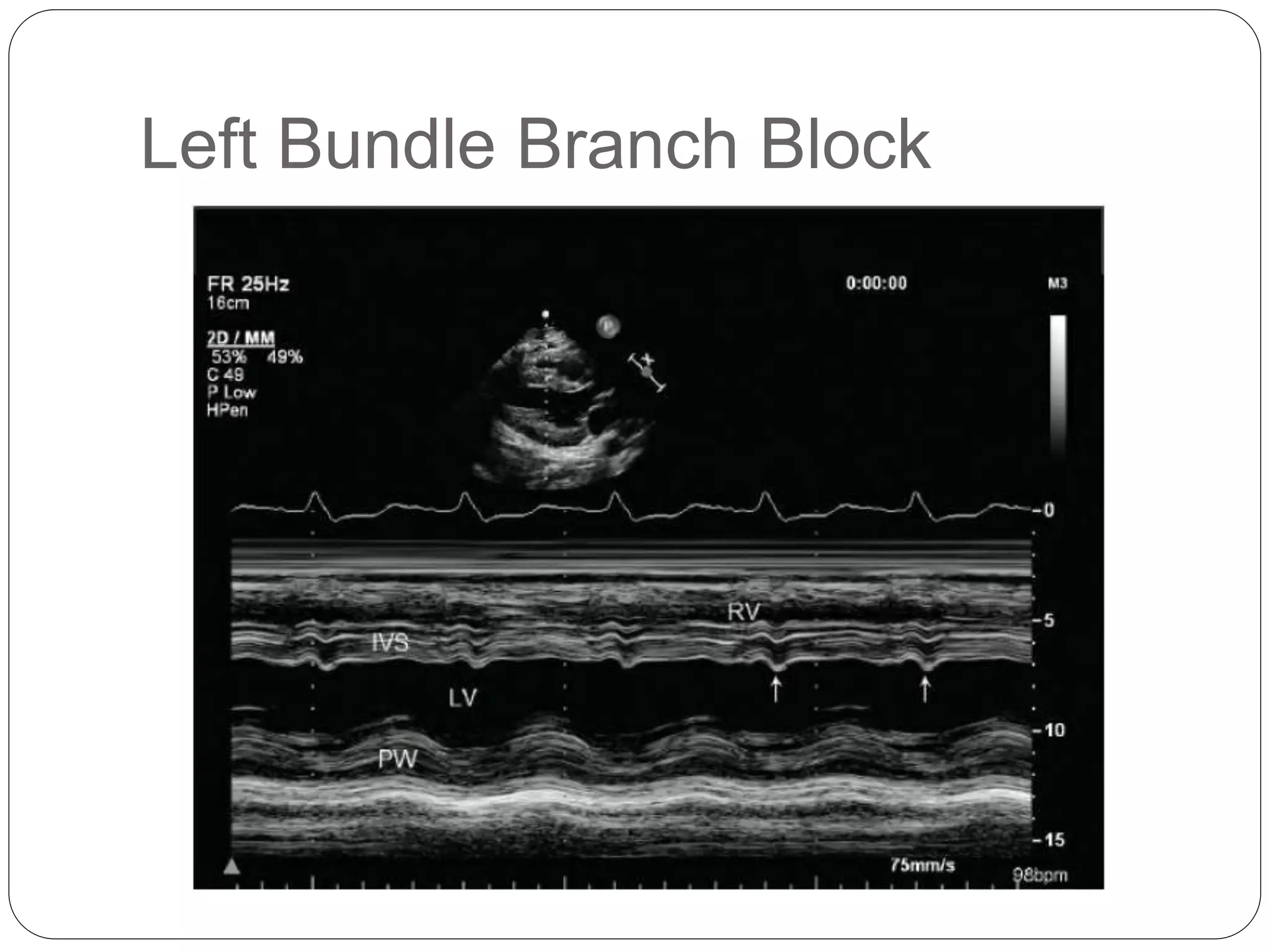
Lv Systolic Function Pptx This review proposes a pocus approach designed to integrate different qualitative and semi quantitative measurements of lv systolic function, to improve the proficiency in cardiac. In this chapter, the authors will describe how to use pocus to estimate cardiac output non invasively which would be pivotal in the diagnosis and management of cardiogenic shock.
Comments are closed.