Patient Experience Mbqip
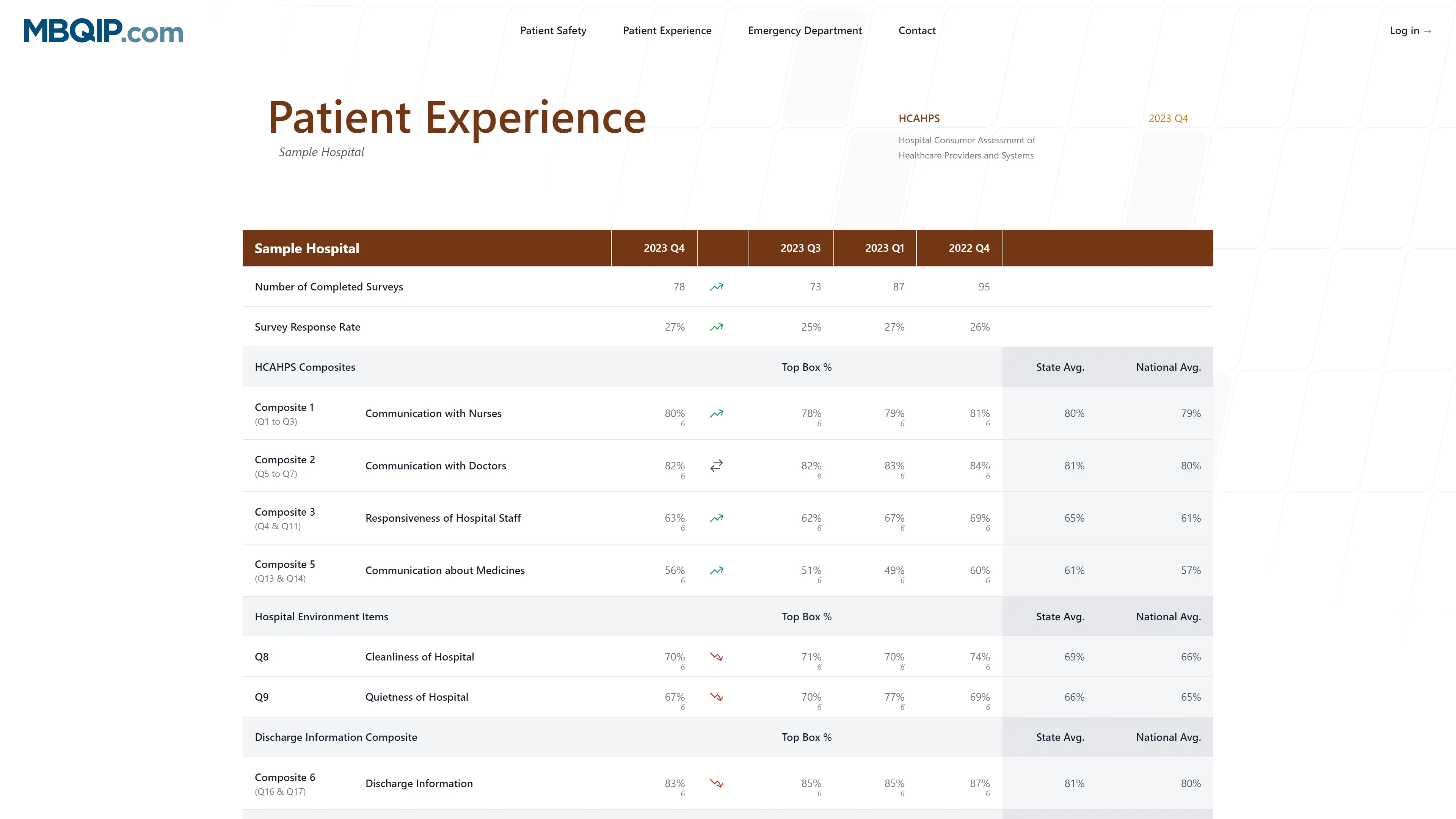
Patient Experience Mbqip In addition to four screening and seven demographic questions, the survey includes 21 questions that ask patients for their feedback on a variety of aspects related to their experience as an inpatient in the hospital. These resources focus on quality improvement related to the patient experience including the medicare beneficiary quality improvement project (mbqip) measures under this domain.

Patient Experience Pdf We created the medicare beneficiary quality improvement project (mbqip) to improve the quality of care patients receive in critical access hospitals (cahs) (pdf 1 mb). mbqip focuses these efforts in the 45 states that participate in the medicare rural hospital flexibility (flex) program. To improve the transitions of care from the critical access hospital to other healthcare settings in order to improve patient outcomes. an overview of the mbqip phases and measures. Hcahps is a standardized survey instrument and data collection methodology for measuring patients’ perceptions of their hospital experience. either the hospital or a vendor representing the hospital can implement the survey. This report summarizes reporting rates and performance among u.s. critical access hospitals (cahs) on medicare beneficiary quality improvement project (mbqip) quality measures for 2023.
Mbqip Db Login Hcahps is a standardized survey instrument and data collection methodology for measuring patients’ perceptions of their hospital experience. either the hospital or a vendor representing the hospital can implement the survey. This report summarizes reporting rates and performance among u.s. critical access hospitals (cahs) on medicare beneficiary quality improvement project (mbqip) quality measures for 2023. This guide provides an overview of measures included in the mbqip 2025 measure cores set. this includes information about the data collection, reporting processes and descriptions for each of the measures. These resources focus on quality improvement related to unplanned hospital readmissions and the social drivers that influence patient outcomes. hospital level, all cause, risk standardized readmission measure that focuses on unplanned readmissions 30 days of discharge from an acute hospitalization. Data will continue to be collected going forward. flex programs and hospitals are always welcome to work on additional quality improvement areas in addition to the core set. this includes, but is not limited to, those listed below. Quality measures: mbqip focuses on a set of measures aligned with national healthcare priorities, including patient safety, patient engagement, care transitions, and outpatient measures. these measures address areas such as emergency department care, inpatient care, and patient experience.

Mbqip Awards This guide provides an overview of measures included in the mbqip 2025 measure cores set. this includes information about the data collection, reporting processes and descriptions for each of the measures. These resources focus on quality improvement related to unplanned hospital readmissions and the social drivers that influence patient outcomes. hospital level, all cause, risk standardized readmission measure that focuses on unplanned readmissions 30 days of discharge from an acute hospitalization. Data will continue to be collected going forward. flex programs and hospitals are always welcome to work on additional quality improvement areas in addition to the core set. this includes, but is not limited to, those listed below. Quality measures: mbqip focuses on a set of measures aligned with national healthcare priorities, including patient safety, patient engagement, care transitions, and outpatient measures. these measures address areas such as emergency department care, inpatient care, and patient experience.
Comments are closed.