Credentialing Vs Contracting Whats The Difference %f0%9f%a4%94%f0%9f%a4%b7%e2%99%80%ef%b8%8f%f0%9f%a4%b7 Insurancetips Providers Credentialing
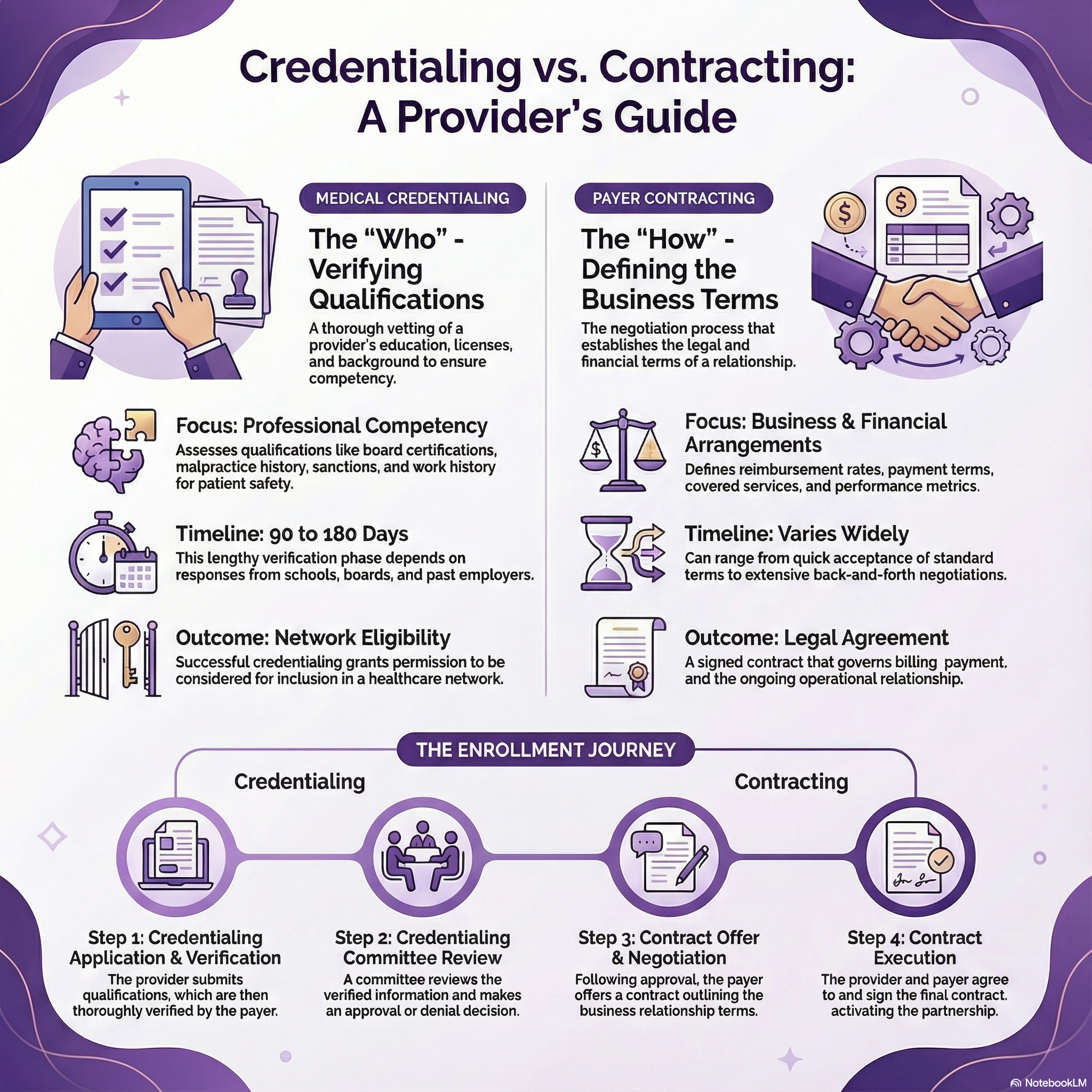
Credentialing Vs Contracting Providers Guide Infographic Medwave Healthcare providers must approach credentialing and contracting as complementary but distinct strategic activities. successful credentialing enables network participation, while effective contracting ensures sustainable business relationships. Credentialing involves verifying your identity and qualifications. contracting is becoming "in network" or a "participating provider" with an insurance payer.

Credentialing Vs Contracting Once credentialing is complete, the next step is insurance contracting, where providers negotiate terms with insurance companies. this process establishes payment agreements, reimbursement policies, and service terms to ensure fair compensation. Credentialing simply verifies the legitimacy of a provider but does not necessarily allow for payment from an insurance payer, as it does not connect your group to a fee schedule. Credentialing almost always precedes contracting, as insurance companies and healthcare networks require verified provider credentials before entering into business relationships. What's the difference?credentialing and contracting are two separate but related processes that healthcare providers must go through to enroll with an insurance company. to contract with an insurance company, a healthcare provider must first be credentialed by that insurance company.

Credentialing Vs Contracting What S The Difference Inlera Credentialing almost always precedes contracting, as insurance companies and healthcare networks require verified provider credentials before entering into business relationships. What's the difference?credentialing and contracting are two separate but related processes that healthcare providers must go through to enroll with an insurance company. to contract with an insurance company, a healthcare provider must first be credentialed by that insurance company. Medical credentialing and contracting are among the essential processes for any healthcare organization in the modern world. however, only a small percentage of healthcare workers know that contracting and credentialing are two distinct concepts requiring completely different procedures. Credentialing is step one. contracting is step two. you need both before you can bill at in network rates. credentialing is the verification step. the insurance company confirms your education, licensure, npi, training, malpractice history, and work experience. Contracting and credentialing are two key processes that ensure healthcare providers and organizations deliver quality, compliant, and safe services. while contracting sets the terms for business relationships, credentialing ensures that providers meet the necessary qualifications. Credentialing ensures that your providers are qualified to deliver care, while contracting establishes the terms under which you get reimbursed. managing both processes effectively enhances your clinic's reputation, streamlines operations, and ensures financial stability.

Credentialing Vs Contracting Know The Difference Medical credentialing and contracting are among the essential processes for any healthcare organization in the modern world. however, only a small percentage of healthcare workers know that contracting and credentialing are two distinct concepts requiring completely different procedures. Credentialing is step one. contracting is step two. you need both before you can bill at in network rates. credentialing is the verification step. the insurance company confirms your education, licensure, npi, training, malpractice history, and work experience. Contracting and credentialing are two key processes that ensure healthcare providers and organizations deliver quality, compliant, and safe services. while contracting sets the terms for business relationships, credentialing ensures that providers meet the necessary qualifications. Credentialing ensures that your providers are qualified to deliver care, while contracting establishes the terms under which you get reimbursed. managing both processes effectively enhances your clinic's reputation, streamlines operations, and ensures financial stability.
Comments are closed.