Credentialing Process Pptx

The Credentialing Process The document outlines the provider credentialing process in the healthcare industry, highlighting the steps involved from application submission to re credentialing. Streamline your understanding of the credentialing process with our comprehensive, fully editable powerpoint presentations. customize to fit your needs and enhance your training sessions effectively.

Credentialing Process An Easy 5 Step Process For 2025 The expedited approval process may not be used if the applicant's application meets one of the criteria listed below, it must be presented to the full board for approval. Join expert cati harris, cbcs, for an information packed webinar on the provider credentialing process. learn the proven method with payer specifics and get a detailed, comprehensive step by step guide. For instance, organizations can create comprehensive ppt templates that outline the credentialing requirements, procedures, and timelines, making it easier for applicants to navigate the process. Credentialing requirements are defined for each organization in a series of documents. these include medical staff bylaws, policies and procedures, rules and regulations. in this section we will discuss those documents and how they support the credentialing process. medical staff governance documents.
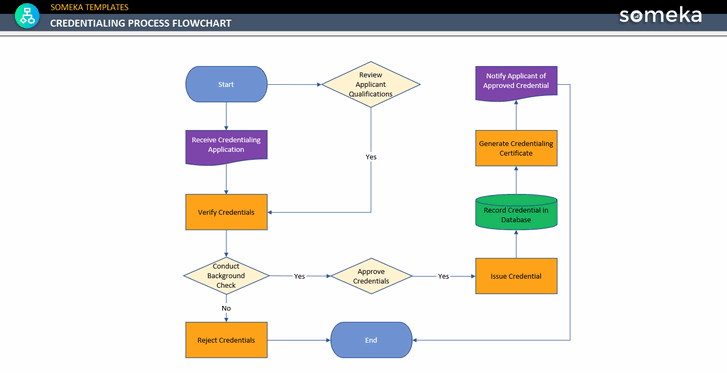
Credentialing Process Flow Chart Free Download For instance, organizations can create comprehensive ppt templates that outline the credentialing requirements, procedures, and timelines, making it easier for applicants to navigate the process. Credentialing requirements are defined for each organization in a series of documents. these include medical staff bylaws, policies and procedures, rules and regulations. in this section we will discuss those documents and how they support the credentialing process. medical staff governance documents. Credentialing, privileging, and enrollment collectively play an important role in verifying healthcare providers' qualifications, assessing their competency, and ensuring inclusion in insurance networks. Med advantage is a credential verification organization that streamlines the costly credentialing process for healthcare providers through automation and a comprehensive database of over 970,000 verified records. There are four phases to this process which will assist the msp and medical staff leadership in evaluating their structure, processes, and outcomes related to credentialing and privileging. Contracting takes an average of 3 6 months, while credentialing takes an average of 60 120 days. these processing times are only average estimates – actual processing times may be quicker or slower.
Comments are closed.